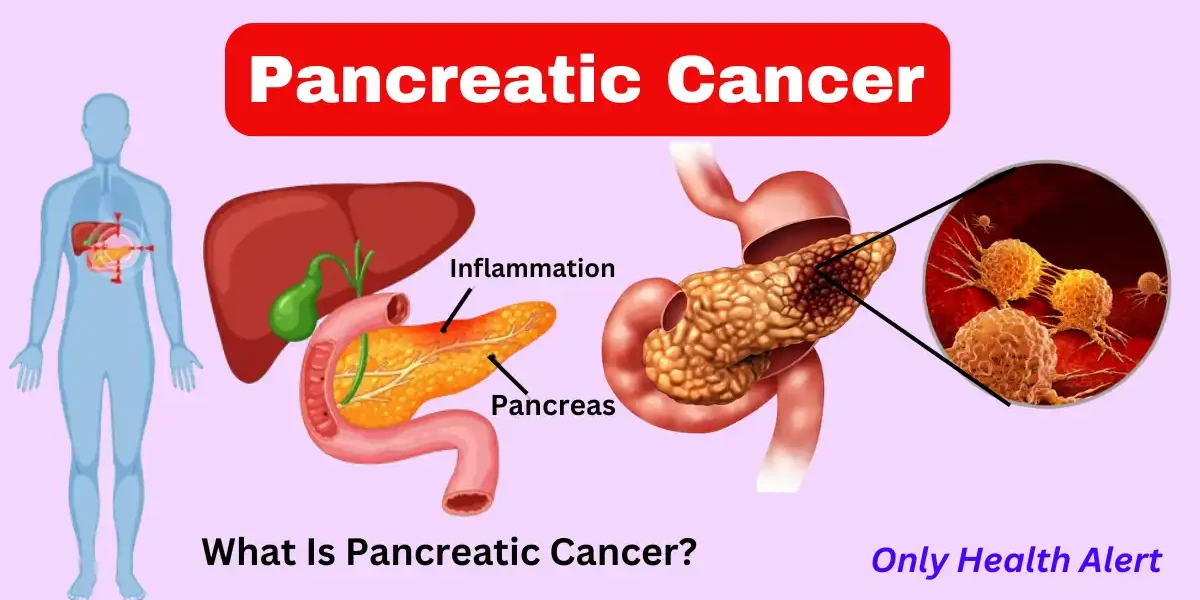
Pancreatic cancer is one of the most aggressive and challenging cancers to treat, often diagnosed at an advanced stage when treatment options are limited. Understanding what pancreatic cancer is, its symptoms, causes, and treatment options can help in early detection and better management.
The pancreas is an organ situated behind the stomach that is essential for aiding digestion and managing blood glucose levels. Pancreatic cancer develops when irregular cells multiply rapidly within the pancreas, resulting in the formation of a tumor.
This cancer is particularly dangerous because it often spreads silently, with symptoms appearing only at an advanced stage. According to the American Cancer Society, pancreatic cancer accounts for about 3% of all cancers but is responsible for 7% of cancer deaths due to its aggressive nature.
Pancreatic cancer is not a single disease but rather a group of malignancies that develop in different parts of the pancreas. The two main categories are exocrine tumors (the most common) and neuroendocrine tumors (rare but often less aggressive). Understanding these types is crucial because they behave differently, require distinct treatments, and have varying prognoses.
Most pancreatic cancers (approximately 95%) are exocrine tumors, which arise from the cells that produce digestive enzymes. The most common subtype is pancreatic ductal adenocarcinoma (PDAC), accounting for 85-90% of all pancreatic cancers.
Pancreatic Ductal Adenocarcinoma (PDAC):
Originates in the ducts that carry digestive enzymes to the small intestine.
Highly aggressive, often spreading before symptoms appear.
Symptoms include jaundice, abdominal pain, and weight loss due to blocked bile ducts or tumor pressure.
Prognosis is generally poor, with a 5-year survival rate of only 10% even with treatment.
Other Rare Exocrine Tumors:
Acinar Cell Carcinoma: Forms in the enzyme-producing cells (acinar cells). Less common (1-2% of cases) but may cause excess enzyme release, leading to fat necrosis (tissue damage).
Squamous Cell Carcinoma: Extremely rare, composed entirely of squamous cells (unlike adenocarcinomas).
Adenosquamous Carcinoma: A mix of adenocarcinoma and squamous cell carcinoma, known for rapid progression.
These tumors are difficult to treat because they are often diagnosed late and resist standard chemotherapy.
Pancreatic neuroendocrine tumors (PNETs), also called islet cell tumors, develop from hormone-producing cells. Unlike exocrine cancers, they tend to grow slower and may even be benign.
Functioning PNETs (Produce Hormones):
Insulinoma: Overproduces insulin, causing low blood sugar (hypoglycemia).
Gastrinoma: Causes excess stomach acid, leading to ulcers (Zollinger-Ellison syndrome).
Glucagonoma: Raises blood sugar, resulting in diabetes-like symptoms and skin rashes.
VIPoma: Triggers watery diarrhea due to vasoactive intestinal peptide (VIP) overproduction.
Non-Functioning PNETs (Do Not Produce Hormones):
More common but harder to detect early since they don’t cause hormonal symptoms.
Often found incidentally during imaging tests.
PNETs have a better prognosis than PDAC, with some patients living years even with metastasis. Treatments include surgery, targeted therapy, and peptide receptor radionuclide therapy (PRRT).
Pancreatic cancer is often called a "silent disease" because early-stage tumors typically cause no noticeable symptoms. By the time symptoms appear, the cancer has often grown or spread, making early detection difficult. However, recognizing the key signs of pancreatic cancer can lead to quicker diagnosis and better treatment outcomes. Here’s a deeper look at the most common symptoms:
One of the most recognizable signs of pancreatic cancer is jaundice, which occurs when a tumor blocks the bile duct, causing a buildup of bilirubin in the blood. This leads to:
Yellow skin and eyes
Dark urine (from excess bilirubin)
Light-colored or greasy stools (due to lack of bile)
Jaundice is more common in cancers located in the head of the pancreas, where the bile duct passes. While jaundice can also result from liver disease or gallstones, its sudden appearance in an otherwise healthy adult should prompt immediate medical evaluation.
A dull, persistent pain in the upper abdomen or mid-back is another hallmark symptom. This happens because the tumor presses against nearby nerves or organs. Unlike temporary stomachaches, pancreatic cancer pain:
Often worsens after eating or lying down
May feel like a deep, gnawing discomfort rather than sharp pain
Can radiate to the back, making some patients mistake it for a muscle strain or spinal issue
Many pancreatic cancer patients experience rapid, unintentional weight loss, even if they haven’t changed their diet. This occurs because:
The tumor interferes with digestion, preventing the body from absorbing nutrients properly.
The cancer itself increases metabolic demand, causing the body to burn calories faster.
Loss of appetite is common, sometimes due to altered taste or early satiety (feeling full quickly).
Since the pancreas produces enzymes that help digest food, tumors can disrupt normal digestion, leading to:
Chronic indigestion or discomfort after meals
Nausea and vomiting, especially if the tumor blocks the stomach’s exit
Bloating and gas due to poor fat breakdown
These symptoms are often mistaken for acid reflux or irritable bowel syndrome (IBS), delaying proper diagnosis.
Pancreatic cancer can suddenly trigger diabetes in people with no prior history. This happens because:
The tumor damages insulin-producing cells.
The body becomes resistant to insulin due to cancer-related changes.
If someone over 50 develops diabetes unexpectedly (without obesity or family history), doctors should consider pancreatic screening.
Chronic fatigue is a common but overlooked symptom. Unlike normal tiredness, cancer-related fatigue:
Doesn’t improve with rest
May be linked to anemia (low red blood cells) or malnutrition
Often accompanies other symptoms like weight loss
Pancreatic cancer increases the risk of abnormal blood clotting, leading to:
Swelling or pain in the legs (DVT)
Sudden shortness of breath (pulmonary embolism)
While blood clots can have many causes, their occurrence alongside other pancreatic cancer symptoms should raise concern.
Vague and common: Symptoms like fatigue, indigestion, or back pain are easily attributed to less serious conditions.
Location of the pancreas: Deep in the abdomen, small tumors don’t press on organs until they grow larger.
No routine screening: Unlike breast or colon cancer, there’s no standard early-detection test for pancreatic cancer.
While the exact cause of pancreatic cancer remains unclear, researchers have identified several key risk factors that increase a person’s likelihood of developing this aggressive disease. Understanding these factors can help individuals assess their risk and take preventive measures where possible.
Pancreatic cancer is most commonly diagnosed in people over 65, with the average age at diagnosis being 71. However, younger individuals can also develop it, especially if they have a family history of the disease. About 5-10% of pancreatic cancer cases are hereditary, linked to inherited genetic mutations such as:
BRCA1 and BRCA2 (also associated with breast and ovarian cancer)
PALB2
Lynch syndrome (HNPCC)
Familial Atypical Multiple Mole Melanoma (FAMMM) syndrome
Those with a strong family history may consider genetic counseling to assess their risk.
Smoking is one of the most significant risk factors, doubling or even tripling the likelihood of pancreatic cancer. Chemicals in tobacco smoke enter the bloodstream, damaging pancreatic cells over time. The good news? Quitting smoking reduces risk—after 10-15 years, an ex-smoker’s risk nearly matches that of a non-smoker.
Long-term inflammation of the pancreas (chronic pancreatitis) significantly raises cancer risk, particularly in cases linked to heavy alcohol use or genetic disorders like hereditary pancreatitis. Additionally, people with long-standing type 2 diabetes have a 1.5 to 2 times higher risk, while sudden-onset diabetes in older adults can sometimes be an early symptom of pancreatic cancer itself.
Studies show that obese individuals (BMI ≥ 30) have a 20% higher risk of pancreatic cancer. Excess body fat promotes inflammation and insulin resistance, which may fuel cancer growth. Dietary habits also play a role:
High consumption of red/processed meats (e.g., bacon, sausages) is linked to increased risk.
Sugary drinks and refined carbs may contribute due to their impact on blood sugar.
Conversely, diets rich in fruits, vegetables, and whole grains appear protective.
Alcohol: Heavy drinking (≥3 drinks/day) can lead to pancreatitis, indirectly raising cancer risk.
Chemical Exposure: Workers exposed to pesticides, dyes, or petrochemicals may face higher risks.
Blood Type: Oddly, people with blood type A, AB, or B have a slightly higher risk than those with type O.
Notably, some patients develop pancreatic cancer without any known risk factors, highlighting the role of random genetic mutations. However, avoiding controllable risks (like smoking and obesity) remains the best strategy for prevention.
Understanding the stages of pancreatic cancer is crucial for determining treatment options and predicting outcomes. Staging helps doctors assess how far the cancer has spread, which directly impacts survival rates and therapeutic approaches. The most commonly used system is the TNM (Tumor, Node, Metastasis) classification, but pancreatic cancer is also grouped into broader stages (0 to IV) for simplicity.
At this earliest stage, abnormal cells are present only in the lining of the pancreas and have not invaded deeper tissues. These cells have the potential to become cancerous but are not yet malignant. Because Stage 0 pancreatic cancer is extremely rare and difficult to detect, most cases are found incidentally during imaging for other conditions. If diagnosed at this stage, surgical removal of the affected tissue can be curative.
Stage I is divided into IA and IB, based on tumor size:
Stage IA: The tumor is 2 cm or smaller and confined to the pancreas.
Stage IB: The tumor is larger than 2 cm but still hasn’t spread beyond the pancreas.
At this stage, the cancer is potentially resectable (removable by surgery), offering the best chance for long-term survival. The Whipple procedure (pancreaticoduodenectomy) or a distal pancreatectomy may be performed, depending on the tumor’s location. Even after successful surgery, adjuvant chemotherapy (such as gemcitabine or FOLFIRINOX) is often recommended to kill any remaining cancer cells.
Stage II is further categorized into IIA and IIB:
Stage IIA: The tumor has grown beyond the pancreas into nearby tissues (like the duodenum or bile duct) but hasn’t reached lymph nodes.
Stage IIB: The cancer has spread to 1-3 nearby lymph nodes but not distant organs.
While Stage II pancreatic cancer is still considered borderline resectable, surgery may be more complex if major blood vessels are involved. Some patients receive neoadjuvant therapy (chemotherapy or radiation before surgery) to shrink the tumor and improve outcomes.
At this stage, the tumor has invaded critical blood vessels (such as the superior mesenteric artery or celiac axis) or extensively spread to nearby lymph nodes. Stage III pancreatic cancer is typically unresectable (inoperable) because removing it would damage vital structures. However, some patients may still benefit from:
Chemotherapy (FOLFIRINOX or gemcitabine + nab-paclitaxel) to control growth.
Radiation therapy to relieve pain or shrink the tumor.
Palliative procedures (like stents to relieve bile duct blockages).
Clinical trials exploring immunotherapy or targeted therapies may also be an option for some patients.
The most advanced stage, Stage IV pancreatic cancer, means the cancer has spread to distant organs such as the liver, lungs, or peritoneum (abdominal lining). At this point, surgery is not curative, and treatment focuses on:
Systemic chemotherapy to slow progression and relieve symptoms.
Pain management (opioids, nerve blocks).
Palliative care to improve quality of life.
The median survival for Stage IV is typically 6 months to a year, though some patients live longer with aggressive treatment.
Diagnosing pancreatic cancer early is challenging because symptoms often appear only in advanced stages. However, doctors use a combination of imaging tests, biopsies, and blood work to confirm the presence of cancer and determine its stage. Below, we explore the key diagnostic methods in detail.
Imaging scans help visualize the pancreas and detect tumors or abnormalities. The most common tests include:
CT (Computed Tomography) Scan – A specialized X-ray that creates detailed cross-sectional images of the pancreas. CT scans help identify tumors, assess their size, and check for spread to nearby organs. A multiphase CT (pancreatic protocol) is often used for better accuracy.
MRI (Magnetic Resonance Imaging) – Uses strong magnetic fields and radio waves to produce high-resolution images. MRCP (Magnetic Resonance Cholangiopancreatography) is a specialized MRI that examines the pancreatic and bile ducts.
PET (Positron Emission Tomography) Scan – Often combined with a CT scan (PET-CT), this test tracks radioactive glucose injected into the body. Cancer cells absorb more glucose, making them visible on the scan. It helps detect metastasis (spread to other organs).
Ultrasound – While less detailed than CT or MRI, an abdominal ultrasound can sometimes spot pancreatic tumors. Endoscopic ultrasound (EUS) is more precise, as it involves inserting a thin, flexible tube with an ultrasound probe down the throat and into the stomach for closer imaging.
These minimally invasive techniques allow doctors to examine the pancreas directly and take tissue samples:
Endoscopic Ultrasound (EUS) – As mentioned, this procedure provides high-resolution images and allows for fine-needle aspiration (FNA), where a small tissue sample is extracted for biopsy.
ERCP (Endoscopic Retrograde Cholangiopancreatography) – A dye is injected into the bile and pancreatic ducts before X-rays are taken. ERCP helps identify blockages caused by tumors and can also place stents to relieve bile duct obstructions.
A biopsy is the only definitive way to confirm pancreatic cancer. Methods include:
Fine-Needle Aspiration (FNA) – Performed during EUS or CT guidance, a thin needle extracts cells from the tumor.
Core Needle Biopsy – A slightly larger needle removes a small tissue cylinder for analysis.
Surgical Biopsy – Rarely used, but if surgery is planned (like a Whipple procedure), a sample may be taken during the operation.
While no blood test can diagnose pancreatic cancer alone, certain markers provide clues:
CA 19-9 – A protein often elevated in pancreatic cancer patients. However, it can also rise due to other conditions (pancreatitis, bile duct obstruction), so it’s not definitive.
CEA (Carcinoembryonic Antigen) – Another marker sometimes used, though less specific to pancreatic cancer.
Liver Function Tests – Abnormal levels may indicate bile duct blockage caused by a tumor.
In some cases, a surgeon may perform a laparoscopy—a small incision in the abdomen to insert a camera and check for cancer spread. This helps determine if the tumor is operable.
Pancreatic cancer is often called a "silent disease" because early-stage tumors rarely cause symptoms. By the time signs like jaundice or abdominal pain appear, the cancer has usually progressed. Additionally, the pancreas is deep inside the abdomen, making small tumors hard to detect on routine exams.
If pancreatic cancer is confirmed, further tests (like genetic profiling) may help guide treatment. Staging scans (CT, MRI, PET) determine whether the cancer is localized, locally advanced, or metastatic, which influences therapy options.
The prognosis of pancreatic cancer depends heavily on the stage at diagnosis, the tumor’s location, and the patient’s overall health. Unfortunately, pancreatic cancer is often diagnosed at an advanced stage, making it one of the deadliest cancers. According to the American Cancer Society, the five-year survival rate for all stages combined is just 12%. However, if the cancer is detected early and remains localized (Stage I), the survival rate improves to 44%. Once the cancer spreads to nearby lymph nodes or tissues (Stage II or III), the five-year survival rate drops to 15%. For metastatic pancreatic cancer (Stage IV), where the disease has spread to distant organs like the liver or lungs, the survival rate is only 3%.
Several factors influence prognosis:
Surgical eligibility: Only 15-20% of patients are candidates for surgery (like the Whipple procedure), which offers the best chance of long-term survival.
Response to treatment: Patients who respond well to chemotherapy (e.g., FOLFIRINOX or gemcitabine) may live longer.
Genetic mutations: Some rare subtypes, like certain neuroendocrine tumors, grow more slowly and have a better outlook.
Overall health: Younger patients with no other major illnesses tend to tolerate aggressive treatments better.
Despite these grim statistics, advancements in targeted therapies, immunotherapy, and early detection techniques are gradually improving outcomes for some patients. Clinical trials also offer hope for new treatments.
The duration of pancreatic cancer—how quickly it progresses and how long patients survive—varies widely based on the stage and treatment.
Early-stage (I & II): Without treatment, the cancer may advance to late-stage within 6–12 months. However, if caught early and surgically removed, some patients survive 5 years or longer.
Locally advanced (Stage III): With chemotherapy and radiation, survival typically ranges from 12–18 months.
Metastatic (Stage IV): At this stage, the average survival is 3–6 months without treatment, but chemotherapy (like FOLFIRINOX) can extend life to 8–12 months or more in some cases.
The disease’s aggressive nature means that even with treatment, most patients survive less than two years after diagnosis. However, exceptions exist—some with slow-growing tumors or exceptional responses to therapy live longer. Palliative care plays a crucial role in managing pain, improving quality of life, and sometimes extending survival by preventing complications like infections or malnutrition.
Pancreatic cancer is notoriously difficult to treat, but advances in medicine have improved survival rates and quality of life for some patients. The choice of pancreatic cancer treatment and medication depends on the cancer’s stage, location, overall health, and genetic factors. Below, we explore the most common and emerging therapies in detail.
Surgery offers the best chance for a cure, but only 15-20% of patients are eligible because the disease is often detected late. The type of surgery depends on the tumor’s location:
Whipple Procedure (Pancreaticoduodenectomy): The most common surgery for tumors in the head of the pancreas. Surgeons remove the pancreatic head, part of the small intestine, gallbladder, bile duct, and sometimes part of the stomach. Recovery is lengthy, but studies show a 5-year survival rate of 20-25% when combined with chemotherapy.
Distal Pancreatectomy: Used for tumors in the body or tail of the pancreas. The surgeon removes the affected portion, sometimes along with the spleen.
Total Pancreatectomy: Rarely performed, this removes the entire pancreas, leading to lifelong diabetes and digestive enzyme dependence.
Post-surgery challenges include managing diabetes (if insulin-producing cells are lost) and digestive issues (requiring enzyme supplements like Creon).
Chemotherapy involves medications that destroy cancer cells or prevent them from multiplying. It can be given:
Before surgery (neoadjuvant therapy) to shrink tumors.
After surgery (adjuvant therapy) to kill remaining cancer cells.
For advanced cancer to slow progression and relieve symptoms.
Common Chemotherapy Regimens:
Gemcitabine (Gemzar): A standard treatment, often combined with nab-paclitaxel (Abraxane), improving survival by several months.
FOLFIRINOX: A powerful combination of 5-FU, leucovorin, irinotecan, and oxaliplatin—used for healthier patients with advanced cancer. It can extend life but has significant side effects (fatigue, neuropathy, diarrhea).
Capecitabine (Xeloda): Sometimes used after surgery or with radiation.
Newer drugs like Irinotecan liposome (Onivyde) are also being tested in clinical trials.
Radiation uses high-energy beams to destroy cancer cells. It’s often combined with chemotherapy (chemoradiation) in cases where:
The tumor is locally advanced (spread to nearby blood vessels but not distant organs).
Surgery isn’t an option.
There’s a need to shrink the tumor before surgery.
Types of Radiation:
External Beam Radiation (EBRT): The most common type, targeting the tumor precisely.
Stereotactic Body Radiotherapy (SBRT): Delivers high doses in fewer sessions, useful for small tumors.
Side effects include fatigue, nausea, and skin irritation.
These newer treatments focus on specific genetic mutations or the immune system:
Targeted Therapy:
PARP Inhibitors (Olaparib/Lynparza): For patients with BRCA gene mutations, these drugs block cancer cell repair mechanisms.
EGFR Inhibitors (Erlotinib/Tarceva): Used with gemcitabine in some advanced cases.
Immunotherapy:
Pembrolizumab (Keytruda): Works for the rare MSI-High (microsatellite instability-high) tumors, helping the immune system attack cancer.
Clinical Trials: Many experimental immunotherapies (like CAR-T cell therapy) are being tested.
For advanced pancreatic cancer, treatment focuses on relieving symptoms rather than curing the disease:
Pain control: Opioids, nerve blocks, or celiac plexus neurolysis (alcohol injection to numb abdominal nerves).
Biliary stents: If the tumor blocks bile flow, a stent keeps the duct open, reducing jaundice.
Nutritional support: Enzyme supplements and dietary adjustments help with digestion.
Research is ongoing to improve outcomes, including:
Personalized medicine (matching treatments to genetic profiles).
Vaccine therapy (stimulating the immune system against cancer cells).
Nanotechnology (delivering drugs directly to tumors).
Patients are encouraged to explore clinical trials, which may offer access to cutting-edge therapies.
While pancreatic cancer cannot always be prevented, certain lifestyle changes and proactive health measures can significantly reduce the risk. Since early detection is rare, prevention plays a crucial role in combating this aggressive disease. Here’s what research suggests:
Avoid Smoking: Tobacco use is one of the strongest risk factors, doubling or even tripling the likelihood of developing pancreatic cancer. Quitting smoking at any age lowers the risk over time.
Maintain a Healthy Weight: Obesity, particularly abdominal fat, increases inflammation and insulin resistance, which may contribute to pancreatic cancer. A balanced diet and regular exercise can help maintain a healthy weight.
Eat a Nutrient-Rich Diet: Studies indicate that diets high in processed meats, sugary foods, and fried foods may elevate risk, while fruits, vegetables, whole grains, and lean proteins may have protective effects. Antioxidant-rich foods like berries, leafy greens, and nuts are particularly beneficial.
Limit Alcohol Consumption: Heavy alcohol use can lead to chronic pancreatitis, a known risk factor for pancreatic cancer. Moderate drinking (one drink per day for women, two for men) is advised.
Manage Diabetes and Chronic Pancreatitis: People with long-standing diabetes or pancreatitis should work closely with their doctors to monitor pancreatic health, as these conditions increase cancer risk.
Genetic Counseling for High-Risk Individuals: Those with a family history of pancreatic cancer or inherited syndromes (like BRCA mutations, Lynch syndrome, or familial atypical mole-malignant melanoma syndrome) should consider genetic testing and regular screenings.
Although no method guarantees prevention, these steps can lower risk and improve overall health, making them worthwhile for everyone.
Pancreatic cancer often leads to severe complications, especially in advanced stages, due to the tumor’s location and its impact on digestion, hormone regulation, and nearby organs. Some of the most common complications include:
Jaundice and Bile Duct Blockage: When a tumor presses on the bile duct, bile cannot flow properly, leading to yellowing skin, dark urine, and itchy skin. A stent may be placed to relieve the blockage.
Severe Pain: Tumors can press on nerves or spread to surrounding tissues, causing debilitating abdominal or back pain. Pain management often requires medications, nerve blocks, or radiation therapy.
Weight Loss and Malnutrition: Since the pancreas aids digestion, cancer can disrupt enzyme production, leading to poor nutrient absorption. Patients may need pancreatic enzyme supplements and nutritional support.
Diabetes Development or Worsening: If the tumor damages insulin-producing cells, new-onset diabetes or uncontrolled blood sugar may occur, requiring careful monitoring.
Blood Clots (Deep Vein Thrombosis - DVT): Pancreatic cancer increases clotting risks, leading to painful swelling or life-threatening pulmonary embolism. Blood thinners may be prescribed.
Bowel Obstruction: Advanced tumors can block the intestines, causing nausea, vomiting, and inability to eat. Surgery or stents may be needed to open the passage.
Liver Failure (If Metastasized): When cancer spreads to the liver, it can impair liver function, leading to fluid buildup, confusion, and fatigue.
Managing these complications requires a multidisciplinary approach, including oncology, pain specialists, nutritionists, and palliative care teams, to improve quality of life.
The survival time for pancreatic cancer varies depending on the stage at diagnosis. Early-stage patients who receive surgery and treatment may live several years, while advanced cases often have a shorter prognosis. On average, the 5-year survival rate is around 12%, but many people with advanced pancreatic cancer live for only a few months without treatment. With aggressive treatment, some patients live longer.
Risk factors for pancreatic cancer include smoking, chronic pancreatitis, obesity, diabetes, family history of pancreatic cancer, age over 60, and certain genetic mutations. People with Lynch syndrome or BRCA mutations are also at higher risk. Men and African Americans have a slightly higher incidence.
While pancreatic cancer is one of the most challenging cancers to treat, it can be beaten in some cases, especially if detected early. Surgery, chemotherapy, radiation, and targeted therapies can lead to remission. However, most cases are diagnosed late, which makes long-term survival more difficult.
Yes, it is possible to live without a pancreas, though it requires lifelong medical management. After complete removal (a total pancreatectomy), a person will need insulin for diabetes and pancreatic enzyme supplements to aid digestion. Lifestyle changes and close medical monitoring are essential.
Several organs can be removed without causing death. These include the spleen, gallbladder, appendix, one kidney, one lung, and reproductive organs like the uterus or testicles. Though some functions are lost, the body can often adapt or be supported through medication or therapy.
Yes, pancreas transplants are possible and are most often done for people with type 1 diabetes who have severe complications. A pancreas transplant can restore insulin production, potentially curing diabetes. However, it requires lifelong use of immunosuppressants to prevent organ rejection.
The heart is the organ that never stops working. It continuously pumps blood throughout the body from before birth until death. It is vital for delivering oxygen and nutrients to tissues and removing waste products.
Several organs can remain viable for transplantation after death, including the kidneys, liver, heart, lungs, pancreas, and intestines. These organs can be donated if removed within a specific time after death, depending on conditions and preservation.
Failure of major organs such as the heart, brain, liver, kidneys, or lungs can lead to death if not treated. Multi-organ failure, where several systems stop functioning, often occurs in critical illness or at the end of life and is typically fatal.
Dialysis is generally not painful, though some patients may feel discomfort from the needle insertion or muscle cramps during treatment. Fatigue, low blood pressure, or nausea can also occur. Most people tolerate dialysis well with proper care.
Typically, the liver and kidneys are among the first organs to fail during the dying process, especially in critical illness. Eventually, the heart and lungs stop, followed by brain activity. The order may vary depending on the cause of death.
An end organ is a target organ that is affected by disease or injury, often in the context of systemic conditions. Examples include the kidneys in hypertension, the eyes in diabetes, and the brain during shock. End organ damage often indicates severe illness and may result in permanent dysfunction.
Pancreatic cancer remains a formidable disease, but awareness of its symptoms, risk factors, and treatment options can lead to earlier detection and better outcomes. Research is ongoing, with immunotherapy and genetic testing offering new hope.
If you or a loved one experiences persistent pancreatic cancer symptoms and signs, consult a doctor promptly. Early action could make all the difference.