Osteoarthritis (OA) is the most common form of arthritis, affecting millions of people worldwide. Often referred to as "wear-and-tear" arthritis, it occurs when the protective cartilage that cushions the ends of bones wears down over time, leading to pain, stiffness, and reduced joint mobility. While osteoarthritis can affect any joint, it frequently targets the knees, hips, hands, and spine.
In this comprehensive guide, we’ll explore osteoarthritis in detail, with a special focus on knee osteoarthritis—its types, symptoms, causes, stages, diagnosis, treatment, and prevention. Whether you’re newly diagnosed or seeking ways to manage joint health, this article provides valuable insights to help you understand and navigate this condition.
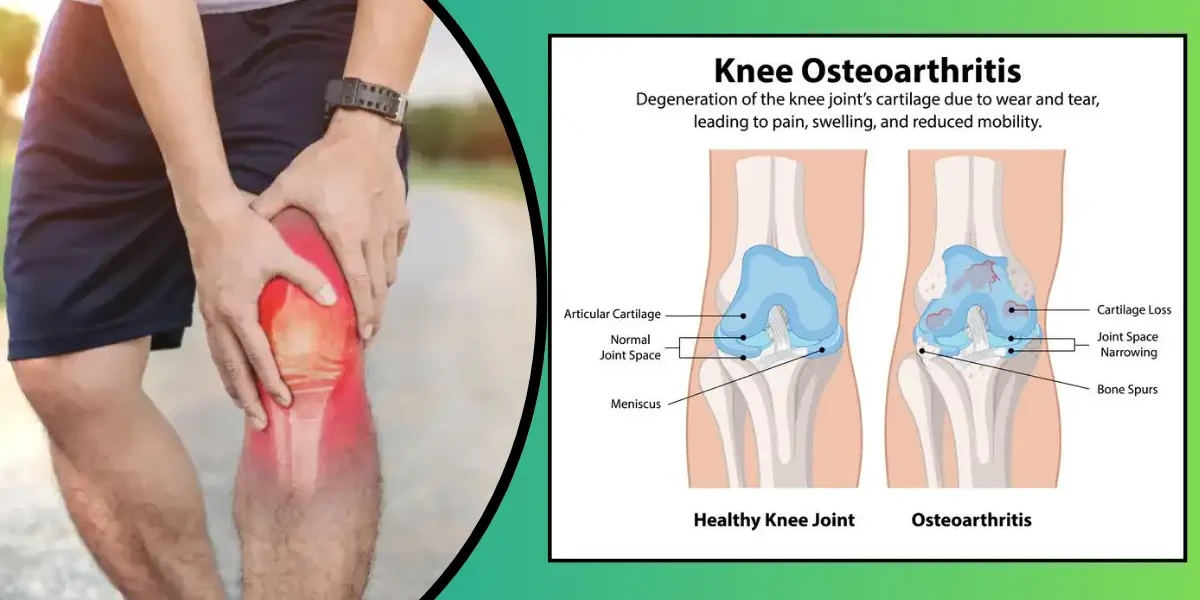
Knee osteoarthritis (OA) is a degenerative joint disease characterized by the gradual breakdown of cartilage—the smooth, cushioning tissue that covers the ends of bones in the knee joint. Over time, this cartilage wears away, leading to bone-on-bone friction, inflammation, and structural changes in the joint. Unlike inflammatory arthritis (such as rheumatoid arthritis), knee osteoarthritis is primarily caused by mechanical wear-and-tear, aging, or injury.
This condition is one of the leading causes of chronic knee pain and disability, especially in adults over 50. However, younger individuals can also develop knee OA due to sports injuries, obesity, or genetic factors. The progression of knee osteoarthritis varies—some people experience mild discomfort for years, while others may face rapid joint deterioration and severe mobility limitations. Early intervention, including weight management, physical therapy, and medication, can help slow its progression and improve quality of life.
Knee osteoarthritis is broadly categorized into two main types, each with distinct causes and progression patterns:
Primary (Idiopathic) Knee Osteoarthritis
This is the most common form, typically associated with aging and natural wear-and-tear on the joint. As people grow older, the cartilage’s ability to repair itself diminishes, leading to gradual thinning and eventual breakdown. Primary OA often affects both knees symmetrically and progresses slowly over decades. While age is the biggest risk factor, genetics also play a role—some people inherit weaker cartilage or joint structures that make them more susceptible.
Secondary Knee Osteoarthritis
Unlike primary OA, secondary osteoarthritis has a clear underlying cause. It can develop at any age due to factors such as:
Joint Injuries – Previous fractures, ligament tears (like an ACL injury), or meniscus damage can destabilize the knee, accelerating cartilage wear.
Obesity – Excess body weight increases stress on knee joints, speeding up cartilage breakdown.
Metabolic Disorders – Conditions like diabetes or hemochromatosis (excess iron) can damage joint tissues.
Congenital or Developmental Abnormalities – Misaligned knees (e.g., bowlegs or knock-knees) create uneven pressure on cartilage.
Inflammatory Joint Diseases – Gout, septic arthritis, or autoimmune diseases can trigger secondary OA.
Understanding whether knee osteoarthritis is primary or secondary helps doctors tailor treatment strategies more effectively. For instance, secondary OA may require addressing the root cause (e.g., weight loss for obesity-related OA or surgery for a malaligned joint), while primary OA focuses more on symptom management and slowing degeneration.
Knee osteoarthritis develops gradually, and its symptoms often start mild before worsening over time. Early detection of these indicators leads to more successful management of the disorder. Below is a deeper exploration of the key symptoms and what they mean.
1. Pain: The Most Common Symptom
Pain is the hallmark of knee osteoarthritis. Initially, it may only occur after prolonged activity, such as walking long distances or climbing stairs. Over time, the pain can become more persistent, even flaring up during rest. Some people describe it as a dull, aching discomfort, while others experience sharp, stabbing pains—especially when putting weight on the joint. Changes in weather, particularly cold or humid conditions, can also intensify the pain for some individuals.
2. Stiffness: Reduced Flexibility in the Joint
Stiffness is another major symptom, often most noticeable after periods of inactivity. Many people with knee osteoarthritis report significant stiffness first thing in the morning, which may last for 30 minutes or longer. Sitting for extended periods (like during a long car ride or movie) can also cause the knee to feel "locked up," making it difficult to move until the joint loosens with gentle motion.
3. Swelling: Inflammation and Fluid Buildup
As the cartilage wears down, the knee may become inflamed, leading to visible swelling. This swelling can be due to two main causes:
Synovitis – Inflammation of the joint lining, causing excess fluid production.
Bone Spurs (Osteophytes) – Extra bone growth that irritates surrounding tissues.
The knee may feel warm to the touch and appear puffy, making it uncomfortable to bend or straighten fully.
4. Reduced Mobility: Difficulty Moving the Knee
As osteoarthritis progresses, the knee’s range of motion diminishes. People may struggle with activities that require full knee extension or flexion, such as squatting, kneeling, or even getting in and out of a car. Some notice that their knee doesn’t straighten completely, leading to a slightly bent posture when standing or walking.
5. Creaking or Popping Sounds (Crepitus)
A grinding or crackling sensation when moving the knee—known as crepitus—is a common sign of advanced osteoarthritis. This occurs because the smooth cartilage that normally cushions the joint has worn away, causing rough bone surfaces to rub together. While crepitus isn’t always painful, it can be unsettling and is often accompanied by stiffness.
6. Weakness or Instability: The Knee "Giving Way"
Muscle weakness around the knee joint is common in osteoarthritis, as pain leads to reduced activity. This can cause feelings of instability, as if the knee might buckle unexpectedly. Some people compensate by shifting their weight to the unaffected leg, which can lead to imbalances and further strain on other joints (like the hips or lower back).
7. Deformities: Changes in Knee Structure
In late-stage osteoarthritis, the joint may start to deform. This can result in:
Bowlegs (Varus deformity) – The knees curve outward.
Knock-knees (Valgus deformity) – The knees angle inward.
These changes occur due to uneven cartilage loss and bone remodeling, altering the knee’s alignment.
If knee pain persists for more than a few weeks, interferes with daily activities, or is accompanied by significant swelling or locking, it’s important to seek medical advice. Early intervention can help slow disease progression and improve long-term outcomes.
Knee osteoarthritis develops when the protective cartilage that cushions the knee joint gradually wears away, leading to pain, stiffness, and reduced mobility. While aging is the most common cause, several other factors contribute to this degenerative condition. Understanding these causes and risk factors can help in prevention and early intervention.
1. Age: The Leading Factor
As we age, the cartilage in our joints naturally begins to break down due to decades of use. Over time, the knee joint’s ability to repair itself diminishes, leading to thinning cartilage, bone spur formation, and joint inflammation. While osteoarthritis can occur in younger individuals, it most commonly affects people over 50.
2. Obesity: Excess Weight Puts Stress on Joints
Carrying extra body weight significantly increases the risk of knee osteoarthritis. For every pound of body weight, the knee experiences about four pounds of pressure during movement. This means that someone who is 20 pounds overweight adds nearly 80 pounds of additional stress to their knees with each step. Over time, this excess strain accelerates cartilage breakdown, making weight management a crucial factor in prevention.
3. Previous Joint Injuries: Trauma Increases Risk
A history of knee injuries—such as fractures, ligament tears (like an ACL injury), or meniscus damage—raises the likelihood of developing osteoarthritis later in life. Even if the injury was treated successfully, the structural changes in the joint can lead to uneven wear and tear, eventually causing cartilage degeneration. Athletes and manual laborers are particularly vulnerable due to repetitive stress on the knees.
4. Repetitive Stress and Overuse
Jobs or activities that involve frequent kneeling, squatting, heavy lifting, or high-impact movements (like running on hard surfaces) can contribute to early cartilage breakdown. Occupations such as construction work, farming, or professional sports often involve these repetitive motions, increasing the risk of knee osteoarthritis over time.
5. Genetics and Family History
Some people are genetically predisposed to developing osteoarthritis. If a close family member has had knee osteoarthritis, your risk may be higher due to inherited traits that affect cartilage structure, joint alignment, or how your body processes inflammation. Research suggests that certain gene mutations can make cartilage more susceptible to damage.
6. Gender: Women Are More Prone
Females over 50 experience knee osteoarthritis at a greater rate than males of similar age. Hormonal changes, particularly after menopause, may play a role since estrogen helps protect cartilage. Additionally, differences in joint structure and muscle strength between genders may contribute to this increased risk.
7. Bone Deformities and Joint Misalignment
Some people are born with or develop structural abnormalities in their knees, such as bowlegs (varus deformity) or knock-knees (valgus deformity). These misalignments place uneven pressure on certain parts of the joint, leading to faster cartilage wear. Similarly, conditions like rheumatoid arthritis or gout can damage joints and increase osteoarthritis risk.
8. Sedentary Lifestyle: Weak Muscles Lead to Joint Strain
While excessive joint stress is harmful, too little movement can also weaken the muscles that support the knee. Strong quadriceps and hamstrings help absorb shock and stabilize the joint. A sedentary lifestyle leads to muscle loss, reducing joint protection and increasing the likelihood of cartilage damage over time.
9. Metabolic and Inflammatory Conditions
Diseases like diabetes and metabolic syndrome are linked to higher osteoarthritis risk due to chronic inflammation and poor circulation, which can impair cartilage health. Additionally, conditions that cause excessive iron (hemochromatosis) or abnormal bone growth (Paget’s disease) may contribute to joint degeneration.
While some risk factors (like age and genetics) can’t be changed, others—such as weight management, injury prevention, and muscle strengthening—can significantly reduce the likelihood of developing knee osteoarthritis. By understanding these causes and taking proactive steps, you can protect your joints and maintain mobility for years to come.
Knee osteoarthritis (OA) progresses gradually, worsening over time as the cartilage continues to deteriorate. Doctors classify this progression into four distinct stages, each with its own characteristics and symptoms. Understanding these stages helps in early detection, effective treatment planning, and slowing disease progression.
In the earliest stage, the knee joint shows minimal signs of wear. The cartilage may begin to soften, and tiny bone spurs (osteophytes) might develop, though they are usually too small to cause noticeable symptoms. Many people in Stage 1 experience no pain or only mild discomfort after prolonged activity. Because symptoms are subtle, this stage often goes undiagnosed unless detected incidentally through imaging tests. However, early intervention—such as weight management, strengthening exercises, and joint-friendly activities—can help delay further damage.
At this stage, cartilage breakdown becomes more apparent, and bone spurs grow larger. X-rays may reveal slight narrowing of the joint space, indicating thinning cartilage. People with Stage 2 knee OA may start to notice occasional stiffness, especially after sitting for long periods or waking up in the morning. Pain may flare up after strenuous activity but typically subsides with rest. While joint damage is still mild, doctors may recommend lifestyle adjustments, physical therapy, or over-the-counter pain relievers to manage symptoms and prevent rapid progression.
By Stage 3, cartilage erosion is significant, leading to noticeable joint space narrowing and increased bone spur formation. The synovial fluid that lubricates the joint may also decrease, causing more friction between bones. Symptoms become more persistent, including frequent pain during movement, swelling after activity, and a grating or popping sensation (crepitus). Stiffness may last longer, and some people experience reduced flexibility, making it harder to bend or straighten the knee fully. At this point, doctors often prescribe stronger anti-inflammatory medications, corticosteroid injections, or custom orthotics. If conservative treatments fail, surgical options like arthroscopy may be considered.
This is the most debilitating stage, where cartilage is almost completely worn away, leading to bone-on-bone contact. The joint space is severely narrowed or absent on X-rays, and large bone spurs develop, sometimes causing visible deformities (such as bowlegs or knock knees). Chronic pain occurs even at rest, and mobility becomes severely limited—walking, climbing stairs, or standing for long periods can be extremely difficult. Inflammation and joint instability increase the risk of falls. Treatment options in Stage 4 are more aggressive, often involving joint replacement surgery (partial or total knee arthroplasty) to restore function and relieve pain.
Diagnosing knee osteoarthritis involves a combination of medical history evaluation, physical examinations, and imaging tests. Since symptoms can overlap with other joint conditions, an accurate diagnosis is crucial for effective treatment. Here’s a deeper dive into the diagnostic process:
The first step in diagnosing knee osteoarthritis is a thorough discussion of symptoms and medical history. A doctor will ask about:
The nature of the pain (dull ache vs. sharp, intermittent vs. constant)
When symptoms started and whether they’ve worsened over time
Factors that worsen or relieve pain (e.g., activity, rest, weather changes)
Previous knee injuries, surgeries, or family history of arthritis
During the physical exam, the doctor will:
Check for swelling, warmth, or redness around the knee
Assess the joint’s range of motion (how far it bends and straightens)
Listen for creaking or grinding sounds (crepitus) when moving the knee
Test for tenderness by pressing around the joint
Evaluate muscle strength and stability to rule out ligament or tendon issues
If osteoarthritis is suspected, imaging tests help confirm the diagnosis and determine its severity:
X-rays – The most common diagnostic tool for knee OA. X-rays reveal:
Narrowing of the joint space (indicating cartilage loss)
Bone spurs (osteophytes) that develop as the body tries to repair itself
Subchondral sclerosis (hardening of bone beneath cartilage)
Misalignment or deformities in the joint
Magnetic Resonance Imaging (MRI) – While not always necessary, an MRI provides detailed images of soft tissues, including:
Cartilage damage not visible on X-rays
Meniscus tears (a common issue that can mimic OA symptoms)
Ligament or tendon injuries
Bone marrow lesions (indicating inflammation)
Ultrasound – Less commonly used but can detect synovitis (joint lining inflammation) and fluid buildup.
If swelling is significant, a doctor may perform arthrocentesis, where a small amount of synovial fluid is extracted from the knee joint and analyzed. This helps:
Rule out infections (septic arthritis) or gout (crystals in the fluid)
Check for signs of inflammation (though OA typically has less inflammation than rheumatoid arthritis)
Blood tests aren’t used to diagnose osteoarthritis directly, but they can help exclude other conditions, such as:
Rheumatoid arthritis (RA) – Positive rheumatoid factor or anti-CCP antibodies
Gout or pseudogout – High uric acid levels or calcium crystals
Inflammatory markers – Elevated ESR or CRP may suggest an autoimmune disorder
Since knee OA shares symptoms with other conditions (e.g., meniscus tears, bursitis, or RA), misdiagnosis can lead to ineffective treatments. A proper diagnosis ensures:
Targeted pain management (e.g., NSAIDs vs. disease-modifying drugs for RA)
Appropriate physical therapy or surgical referrals
Lifestyle adjustments (weight loss, activity modifications) to slow progression
If you’re experiencing persistent knee pain, stiffness, or swelling, consult a rheumatologist or orthopedic specialist for a comprehensive evaluation. Early diagnosis can help preserve joint function and improve long-term outcomes.
While osteoarthritis is a chronic condition, its progression varies. Many people manage symptoms effectively with lifestyle changes, medications, and physical therapy. Severe cases may require surgery, but early intervention can delay joint deterioration.
When it comes to managing knee osteoarthritis (OA), treatment focuses on relieving pain, improving joint function, and slowing disease progression. The approach varies depending on the severity of the condition, but a combination of lifestyle changes, medications, therapies, and—in advanced cases—surgery can help patients maintain mobility and quality of life. Below, we explore these options in detail.
1. Lifestyle Modifications
One of the most effective ways to manage knee OA is through weight management and activity adjustments. Excess body weight increases stress on knee joints, accelerating cartilage breakdown. Losing even a small amount of weight (5–10% of body weight) can significantly reduce pain and improve mobility. Low-impact exercises like swimming, cycling, and walking help maintain joint flexibility without worsening damage. Avoiding high-impact activities (e.g., running, jumping) and prolonged kneeling or squatting can also prevent further strain.
2. Physical Therapy and Exercise
A structured physical therapy (PT) program strengthens the muscles around the knee (quadriceps, hamstrings, and calves), providing better joint support. Therapists may recommend:
Strengthening exercises (e.g., leg presses, straight-leg raises)
Range-of-motion stretches to prevent stiffness
Balance and stability training to reduce fall risk
Aquatic therapy, which reduces joint pressure while improving strength
Regular PT can delay the need for surgery and improve daily function.
3. Pain Relief Medications
Medications help control pain and inflammation but do not reverse cartilage damage. Common options include:
Acetaminophen (Tylenol) – Effective for mild to moderate pain but should be used cautiously to avoid liver damage.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) – Such as ibuprofen (Advil) or naproxen (Aleve), which reduce both pain and inflammation. Long-term use can cause stomach ulcers or kidney issues, so doctors may prescribe topical NSAIDs (gels or creams) as a safer alternative.
Duloxetine (Cymbalta) – An antidepressant that also helps with chronic OA pain by altering pain signals in the brain.
4. Joint Injections
For moderate to severe pain that doesn’t respond to oral medications, injections may be recommended:
Corticosteroid Injections – Provide rapid anti-inflammatory relief, often lasting weeks to months. However, frequent use can weaken cartilage, so doctors typically limit them to 3–4 times per year.
Hyaluronic Acid Injections (Viscosupplementation) – A gel-like fluid that lubricates the knee, reducing friction and pain. These may require a series of injections and work best in early to moderate OA.
Platelet-Rich Plasma (PRP) or Stem Cell Therapy – Emerging treatments that may promote cartilage repair, though research on their long-term effectiveness is ongoing.
5. Assistive Devices and Braces
Knee Braces – Unloader braces shift pressure away from damaged areas, while compression sleeves provide mild support and warmth.
Orthotic Shoe Inserts – Can correct alignment issues and reduce knee strain.
Canes or Walkers – Help offload weight from the affected knee during walking.
When conservative treatments fail, surgery may be necessary. Options include:
1. Arthroscopic Surgery
A minimally invasive procedure where a surgeon inserts a tiny camera (arthroscope) to remove loose cartilage, bone spurs, or inflamed tissue. However, this is not recommended for most OA cases unless there’s a specific mechanical issue (e.g., a torn meniscus).
2. Osteotomy
Best for younger patients with early-stage OA on one side of the knee. The surgeon reshapes or realigns the bones to shift weight away from the damaged area, delaying the need for a knee replacement.
3. Partial or Total Knee Replacement (Arthroplasty)
Partial Knee Replacement – Only the damaged compartment of the knee is replaced with metal/plastic implants. Recovery is faster than a full replacement.
Total Knee Replacement (TKR) – The entire joint is replaced with an artificial prosthesis. TKR is highly effective for end-stage OA, with most patients experiencing significant pain relief and restored mobility after rehabilitation.
The best approach depends on factors like:
Disease stage (early vs. advanced)
Age and activity level
Overall health and weight
Personal preferences (e.g., willingness to try injections vs. surgery)
A rheumatologist or orthopedic specialist can help tailor a plan to your needs.
While there’s no cure for knee osteoarthritis, early intervention and a multi-modal treatment plan can dramatically improve comfort and function. If knee pain is affecting your daily life, consult a doctor to explore the best options—whether that’s physical therapy, medications, injections, or surgery.
Knee osteoarthritis may seem inevitable with age, but research shows that smart lifestyle choices can significantly reduce your risk—or at least delay its onset. Here’s a deeper look at evidence-backed prevention methods:
Weight Management: Your Knees’ Best Defense
Every extra pound puts 4 pounds of pressure on your knees when walking—and up to 10 pounds when climbing stairs. Studies confirm that obese adults have 4-5 times higher risk of knee OA. The good news? Losing just 10-15 pounds can cut OA risk in half. Focus on sustainable weight loss through:
A Mediterranean-style diet (rich in fish, olive oil, and vegetables)
Portion control strategies
Low-impact exercises like swimming or cycling
Exercise Smart, Not Hard
While movement is crucial, the wrong type can accelerate damage. The ideal regimen includes:
Strength training (2-3x/week): Target quadriceps, hamstrings, and glutes to stabilize the knee
Low-impact cardio: Water aerobics, elliptical machines, or brisk walking
Flexibility work: Yoga or tai chi to maintain range of motion
Pro Tip: Avoid deep squats, lunges, or plyometrics if you have early OA symptoms.
Joint-Saving Daily Habits
Small adjustments make a big difference:
Wear supportive shoes with cushioning (replace every 300-500 miles)
Use knee pads for gardening/floor work
Practice good posture to avoid uneven weight distribution
Take movement breaks if you sit for long periods
Nutrition for Cartilage Health
Emerging research highlights these nutrients:
Omega-3s (wild salmon, walnuts): Reduce joint inflammation
Vitamin K (kale, spinach): Supports bone density
Collagen peptides: May help cartilage regeneration (studies ongoing)
Turmeric/ginger: Natural anti-inflammatories
Left unchecked, knee OA can trigger a cascade of problems beyond joint pain. Recognizing these complications early allows for better management:
Progressive Deformity
"Bowlegged" (varus) or "knock-kneed" (valgus) alignment develops as cartilage erodes unevenly
Visible joint enlargement from bone spurs
Muscle Atrophy & Weakness
Thigh muscles (quadriceps) may shrink by 20-30% due to reduced activity
Creates dangerous instability, increasing fall risk
Secondary Joint Damage
Compensatory movements overload hips/spine
60% of severe knee OA patients develop hip problems within 5 years
Sleep disruption from chronic pain increases fatigue and depression risk
Social isolation as mobility decreases
Weight gain from activity avoidance worsens OA progression
Acute pseudogout attacks: Sudden, severe swelling when cartilage crystals enter joint fluid
Osteonecrosis: Bone tissue death from compromised blood flow
Rapid progression: Some patients advance from Stage 2 to Stage 4 in <18 months without intervention
Critical Red Flags
✓ Sudden inability to bear weight
✓ Fever with joint swelling (possible infection)
✓ Locked knee that won’t straighten
The Bottom Line: While OA can’t be reversed, today’s treatments—from viscosupplementation injections to personalized rehab programs—can prevent most complications when started early. If your knee pain persists beyond 2 weeks or limits daily activities, consult an orthopedic specialist for a prevention-focused action plan.
Knee osteoarthritis can be effectively controlled with proper care and the right strategies. Early diagnosis, a healthy lifestyle, and proper medical care can significantly improve joint function and reduce pain. If you experience persistent knee discomfort, consult a doctor to explore the best treatment options for your needs.
By understanding what knee osteoarthritis is, its causes, symptoms, and treatments, you can take proactive steps to protect your joint health and maintain an active, pain-free life.
You Might Also Like